
You feel tired but cannot switch off at night. You wake somewhere between 2am and 4am, alert and often anxious, without a clear reason. Weight has appeared around your abdomen that was not there before. You are more reactive than usual, irritated by things that would not normally register. You have tried managing your stress. It helps temporarily. Then the pattern returns.
Our research indicates this is not a willpower problem or a stress management failure. It is a self-reinforcing biological cycle in which elevated cortisol and mineral depletion drive each other, and neither resolves without addressing both.
Do You Recognise This Pattern?
Before the mechanism, a brief check. The following are specific observable signs that people searching this topic consistently report. Read through and note how many apply to you right now.
Energy and Sleep
You wake between 2am and 4am, alert and often anxious, without being able to return to sleep easily.
You feel wired at night but exhausted during the day, as if your body cannot downshift regardless of how tired you are.
You rely on caffeine to function in the morning but it increases your anxiety rather than simply providing energy.
Body and Weight
Weight is accumulating specifically around your abdomen, not evenly distributed across your body.
Your face feels or looks slightly swollen or puffy particularly in the morning.
You retain water and feel bloated without a clear dietary explanation.
Mood and Nervous System
Anxiety arrives before you have a clear reason for it, particularly in the morning or when waking at night.
You are more reactive than usual, irritated by things that would not normally bother you.
A low-level sense of dread or unease that you cannot attribute to a specific cause.
Physical and Cognitive
You get sick more often than you used to, or take longer to recover from illness.
Headaches appear regularly, particularly in the afternoon.
Brain fog and difficulty concentrating despite adequate sleep.
If you recognise five or more of these, the cortisol-mineral depletion cycle described below is very likely the mechanism. If you recognise three or four, it is worth reading the full post before concluding otherwise.
BEFORE YOU READ FURTHER This post describes one specific mechanism behind a cluster of common symptoms: chronic cortisol elevation driving mineral depletion and disrupting the body systems that depend on both. This is a real and common mechanism. It is not the only mechanism that produces these symptoms. See a healthcare provider before treating this as a cortisol-mineral issue if: any symptoms are severe rather than the chronic low-grade pattern described here, you have a diagnosed adrenal, pituitary, or endocrine condition, your weight changes have been significant and rapid, or anxiety or mood symptoms are severely affecting your daily life and relationships. The mechanism described in this post is most relevant for people experiencing a gradual, multi-system, chronic pattern driven by sustained stress without a diagnosed underlying condition. If that is your situation, read on. |

The Cycle in Plain Terms
Research suggests chronic cortisol elevation contributes to magnesium depletion, partly through increased urinary excretion under stress. Magnesium plays a role in the HPA axis feedback mechanism that allows the stress response to stand down after a stressor passes. When magnesium is consistently low, this feedback may be less efficient, contributing to a more reactive and slower-recovering stress response.
DEFINITION HPA AXIS The hypothalamic-pituitary-adrenal axis is the three-part system governing cortisol release. The hypothalamus detects stress and signals the pituitary, which signals the adrenal glands to release cortisol. When magnesium is adequate, a feedback loop returns the system to baseline after the stressor passes. When magnesium is depleted, that feedback loop loses sensitivity and cortisol remains elevated long after the trigger has gone. |
When magnesium is depleted, the feedback fails. Cortisol stays elevated. Elevated cortisol depletes further magnesium. The system cannot self-correct because the raw material that powers the correction mechanism has been consumed.
Cortisol also depletes zinc with each activation. Zinc is required for over 300 enzymatic processes including immune function, testosterone production, and the hormonal balance mechanisms most affected by chronic stress. Zinc deficiency develops as a downstream consequence and adds its own symptom layer on top of the cortisol pattern.
WHAT TO DO ABOUT IT The HPA axis requires two things to regulate properly: a reduced stressor input and the mineral reserves to power its feedback mechanism. The stressor reduction comes first, whether that is reducing workload, addressing the relationship or financial pressure driving the sustained activation, or building genuine recovery windows into the demand cycle. Without that, mineral restoration improves the system’s regulatory capacity but the stressor continues driving elevation. With both: ionic magnesium restored via fulvic acid gives the HPA axis the biological raw material to close the feedback loop more effectively. The morning sipping protocol, dissolving ionic magnesium in a one-litre bottle and sipping from waking until approximately 2pm, supports that capacity through the hours of highest cortisol activation. |
DOES THIS APPLY TO YOU? If you have been under sustained stress for more than four to six weeks rather than responding to a single acute event, the depletion cycle is almost certainly active. A difficult day does not meaningfully deplete magnesium reserves. Months of continuous activation does. If your symptoms have been present for weeks or months and have not responded to rest alone, the mechanism described here is the more likely explanation than acute stress. |
What Elevated Cortisol Does to Sleep
Cortisol follows a natural daily rhythm, lowest around midnight and rising toward a morning peak. When the HPA axis is dysregulated, that rise begins too early and too sharply. It crosses the arousal threshold at approximately 3am. You wake alert and anxious. The overnight mineral depletion that occurs simultaneously removes the GABA buffer that would otherwise absorb the cortisol spike and keep you asleep.
The full 3am mechanism and the restoration protocol are covered in our post on why you wake up at 3am and what the biology actually says.
WHAT TO DO ABOUT IT The morning sipping protocol addresses this at the root. Building a higher ionic mineral baseline throughout the day means the overnight depletion begins from a higher starting point and takes longer to reach the threshold that triggers the 3am wake. A small additional amount of ionic magnesium dissolved in warm water 30 to 60 minutes before sleep supports overnight reserves directly. |
DOES THIS APPLY TO YOU? If your waking is specifically between 2am and 4am and comes with alertness or anxiety rather than a physical need to use the bathroom, this is the cortisol-mineral intersection pattern. If you are waking at other times or for physical reasons, a different mechanism is more likely driving the disruption. |
What Cortisol Does to Your Weight
Cortisol directly stimulates fat storage in the abdominal region through glucocorticoid receptors concentrated in visceral fat tissue. This is not a calories problem. It is a hormonal environment problem. Cortisol is directing fat to that specific location regardless of dietary intake. It also elevates blood sugar to prepare the body for action. When that blood sugar is not used for physical activity, insulin stores it as fat in the same abdominal region.
WHAT TO DO ABOUT IT Dietary restriction alone does not address this because the hormonal environment driving the storage remains active. Lowering the cortisol signal by restoring HPA axis regulation changes the fat storage environment. Ashwagandha has clinical evidence for reducing serum cortisol over four to six weeks, which shifts the glucocorticoid receptor activation driving visceral fat accumulation. |
DOES THIS APPLY TO YOU? If weight is accumulating specifically around your abdomen and is resistant to changes in diet or exercise that would normally produce results, the cortisol mechanism fits. If weight gain is evenly distributed or directly proportional to changes in food intake, the cortisol receptor mechanism is less likely to be the primary driver. If weight change has been significant and rapid rather than gradual, or if it is accompanied by other symptoms such as extreme fatigue, temperature sensitivity, or unexplained hair loss, a thyroid or endocrine assessment is warranted before attributing it to cortisol. Abdominal weight accumulation has multiple causes and cortisol is one of them. |
What Cortisol Does to Your Immunity
Cortisol suppresses immune function as part of the emergency response, diverting energy toward immediate survival and away from long-term maintenance. Chronic elevation means chronic immune suppression. The zinc depletion that follows each cortisol activation compounds this directly: zinc is required for T-cell production, the primary mechanism of the adaptive immune response. The combination produces measurable degradation in immune capacity.
WHAT TO DO ABOUT IT Zinc restoration is the specific requirement here alongside magnesium. Ionic zinc forms have higher bioavailability than the zinc oxide used in many standard supplements. Restoring zinc through more bioavailable forms while addressing the cortisol pattern through adaptogenic support covers both the hormonal suppression signal and the mineral substrate that immunity requires to function. |
DOES THIS APPLY TO YOU? If you are getting sick more frequently than you used to, recovering more slowly, or finding infections recur rather than fully resolving, immune suppression from elevated cortisol is a likely contributor, especially if it coincides with other symptoms in this post. If immune challenges are isolated and not accompanied by the other patterns described here, other factors warrant investigation first. |
What Cortisol Does to Hormonal Balance in Women
Cortisol and progesterone are produced from shared precursor molecules in the steroid hormone pathway. Some researchers propose that under conditions of chronic stress, cortisol synthesis is prioritised in ways that reduce progesterone production. This proposed pathway is sometimes called the pregnenolone steal hypothesis. It is not a mainstream clinical consensus, but it is one framework that researchers use to explain why chronic stress and low progesterone symptoms frequently appear together. What is better established is that chronic HPA axis activation disrupts sex hormone balance broadly, through multiple mechanisms rather than a single one.
DEFINITION PREGNENOLONE STEAL Pregnenolone is a steroid precursor molecule involved in the production of cortisol, progesterone, testosterone, and other hormones. Some researchers propose that under chronic stress, cortisol synthesis draws on pregnenolone in ways that reduce its availability for progesterone production. This hypothesis, sometimes called the pregnenolone steal, is used to explain the co-occurrence of stress and low progesterone symptoms. It remains a proposed mechanism rather than established mainstream endocrinology. The broader observation, that chronic HPA axis activation disrupts sex hormone balance, is well-documented even if the precise mechanism is debated. |
The downstream effects include irregular cycles, worsened PMS, poor sleep in the luteal phase, low mood in the second half of the cycle, and in perimenopause an acceleration of the hormonal fluctuations already occurring. Low progesterone symptoms often appear alongside high cortisol symptoms because they share the same root cause.
WHAT TO DO ABOUT IT Ashwagandha has RCT evidence for reducing cortisol output and perceived stress in adults under chronic stress. This is why it appears in both stress management and women’s hormonal health research. If the stress-driven disruption to progesterone balance is part of the picture, reducing the cortisol load through adaptogenic support addresses the upstream driver while other interventions address the downstream hormonal effects. This is one approach; GP assessment of progesterone levels directly is the appropriate clinical step for significant hormonal disruption. |
DOES THIS APPLY TO YOU? If your symptoms worsen in the second half of your cycle, particularly in the week before menstruation, and have coincided with a period of sustained stress, the stress-driven hormonal disruption pattern described above is worth investigating. If symptoms are consistent across the entire cycle rather than phase-specific, other hormonal mechanisms warrant investigation. If you are in perimenopause or post-menopause, hormonal changes involve multiple overlapping mechanisms and direct testing of oestrogen and progesterone levels is the appropriate first step. GP or gynaecologist assessment is recommended for significant hormonal disruption rather than self-directed supplementation alone. |
What Cortisol Does to Your Mood and Mind
Research associates sustained cortisol elevation with reduced GABA signalling efficiency. GABA is the nervous system’s primary calming signal, and when its function is impaired, the nervous system can become more reactive. Anxiety arrives before there is a clear external reason. Minor irritations produce disproportionate responses. The hippocampus, the brain region most involved in memory and concentration, has a high density of cortisol receptors and research in both animals and humans suggests chronic elevation affects its function. The cognitive and emotional symptoms that accompany chronic stress have a real biological basis, even when they are not visible on a standard clinical assessment.
WHAT TO DO ABOUT IT Magnesium glycinate addresses the mineral side of stress-related anxiety from two directions. Magnesium supports GABA function and the glycine component has its own calming effect on neuronal excitability, with research supporting both. More bioavailable magnesium forms, including glycinate and citrate, are more likely to meaningfully restore cellular magnesium levels than low-absorption forms like oxide. Many people with this pattern report a noticeable improvement in anxiety and sleep quality within one to two weeks of switching to a more bioavailable form. |
DOES THIS APPLY TO YOU? If the anxiety feels biochemical rather than situational, arriving without a clear trigger at predictable times such as morning or 3am, the GABA suppression mechanism is very likely active. If anxiety is consistently tied to specific situations or thoughts, psychological support alongside mineral restoration is a more complete approach. If anxiety is severe, significantly affecting daily function or relationships, or accompanied by panic attacks or intrusive thoughts, that warrants direct assessment and support from a mental health professional regardless of mineral status. Mineral depletion may be a contributing factor. It is not a substitute for clinical mental health support when anxiety is at a clinical level. |
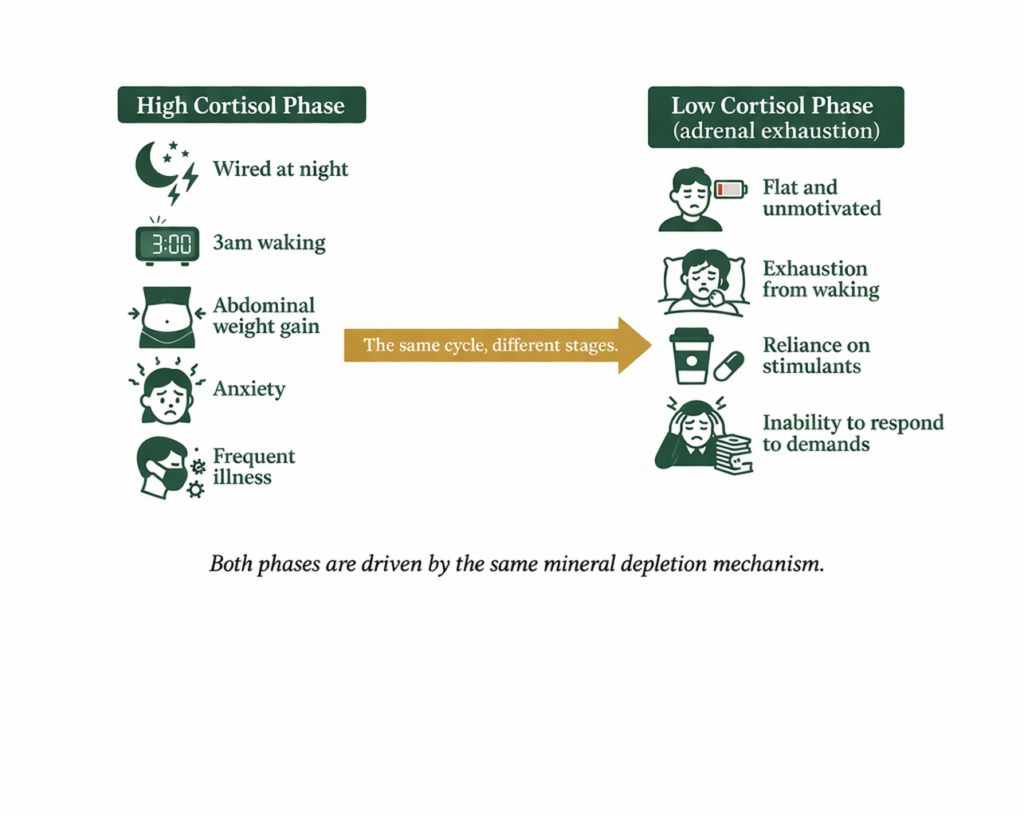
When Cortisol Goes the Other Way
Not everyone in this pattern is experiencing elevated cortisol as the dominant feature. Some people have been in a sustained high-demand state for long enough that the stress response has shifted toward a flatter, lower-output pattern. This is sometimes described as HPA axis dysregulation in the low-output direction. It is not a recognised clinical diagnosis in the same way as conditions like Addison’s disease, but the experience is real and distinct. If you feel flat rather than wired, unmotivated rather than anxious, exhausted from the moment you wake rather than unable to sleep, and dependent on stimulants just to reach baseline function, this lower-output pattern may describe where you are.
WHAT TO DO ABOUT IT The mineral restoration approach is identical regardless of which phase you are in. The adaptogenic approach also applies: ashwagandha modulates the HPA axis rather than simply suppressing or stimulating it, making it relevant across both the elevated and depleted phases of the same cycle. |
DOES THIS APPLY TO YOU? If your symptom pattern shifted over time from wired and anxious to flat and exhausted, you are likely looking at the later stage of the same cycle rather than a separate condition. Both phases require the same mineral foundation to begin recovering. If you have been in the flat and depleted phase for an extended period without any prior history of wired and anxious, other causes of low energy warrant investigation alongside this mechanism. |
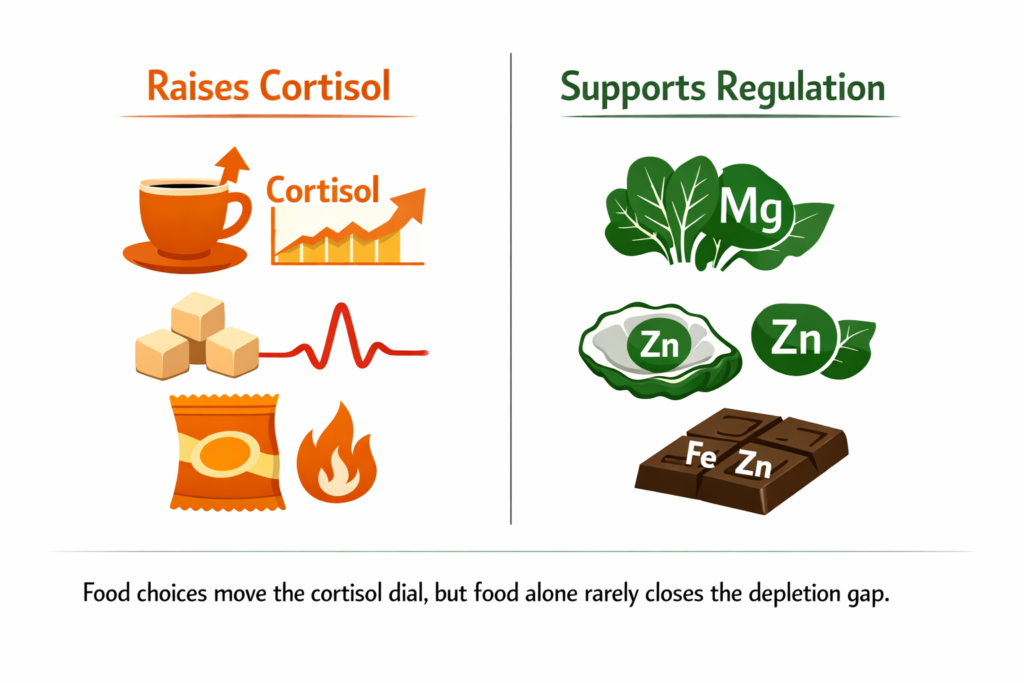
What Foods Raise Cortisol and What Supports Regulation
Caffeine stimulates cortisol release with every dose, extending and amplifying elevation that may already be present. Sugar triggers cortisol through the blood glucose regulation response. Ultra-processed foods produce an inflammatory signal the body reads as a stressor.
What supports regulation: dark leafy greens, seeds, dark chocolate, and legumes provide dietary magnesium. Red meat, oysters, and pumpkin seeds provide zinc. However, modern soil depletion means food sources alone are rarely sufficient for someone with established deficiency from a sustained stress period. Dietary changes support the direction of travel but do not replace ionic mineral supplementation for people in the active depletion cycle.
Standard Thinking vs. The Biological Reality
Standard Thinking | The Biological Reality |
|---|---|
High cortisol is caused by stress | Stress is the primary driver. The mineral depletion from sustained cortisol activation then impairs the feedback loop that should allow the system to stand down, compounding elevation. Both the stressor and the depleted feedback capacity need addressing |
Manage your stress and cortisol will normalise on its own | Stress management addresses the input side and is genuinely effective. Mineral restoration addresses the biological feedback capacity that chronic activation has degraded. Both sides respond better when both are addressed simultaneously |
Cortisol belly fat is just overeating | Visceral fat accumulation in the abdomen is a direct effect of glucocorticoid receptor activation in that tissue, not simply caloric surplus |
Anxiety from stress is psychological | Cortisol-driven anxiety is direct GABA receptor suppression. It is biochemical, not characterological |
Low energy from stress is burnout | Adrenal exhaustion with low cortisol output is a measurable physiological state, not a motivation or discipline problem |
Women’s hormonal disruption from stress is inevitable | The pregnenolone steal is a specific mechanism that is addressable once identified. It is not an inevitable consequence of ageing or stress |
Frequently Asked Questions
What are the most common symptoms of high cortisol?
The most consistently reported symptoms are abdominal weight gain, disrupted sleep with 3am waking, anxiety without a clear trigger, fatigue that does not resolve with rest, frequent illness from immune suppression, brain fog, and mood instability. These appear together because they share one upstream driver: HPA axis dysregulation producing chronically elevated cortisol and the mineral depletion that follows each activation.
What are the symptoms of high cortisol in females specifically?
Women experience all of the general high cortisol symptoms plus specific disruption to sex hormone balance. Research supports an association between chronic HPA axis activation and reduced progesterone, with several proposed mechanisms including effects on shared hormone precursor pathways. This association explains why low progesterone symptoms and high cortisol symptoms frequently appear together. In perimenopause, chronic stress can accelerate and worsen the hormonal fluctuations already occurring. The low progesterone post covers the hormonal picture specifically, and GP assessment of hormone levels directly is the appropriate step for significant cycle disruption.
Can adaptogens lower cortisol naturally?
Yes. Ashwagandha specifically has multiple randomised controlled trials showing reductions in serum cortisol and improvements in self-reported stress scores. The mechanism is modulation of the glucocorticoid receptor pathway, improving HPA axis feedback sensitivity so the body recognises when cortisol is no longer needed and stands down. This is different from sedating the nervous system. Shilajit complements this by restoring the ionic mineral supply the HPA axis requires to regulate cortisol properly.
How long does it take to lower cortisol naturally?
Reduced anxiety and improved sleep typically emerge over two to three weeks as GABA function improves with rising magnesium levels. Meaningful HPA axis regulation improvement typically takes four to six weeks of consistent ionic mineral supplementation and adaptogenic support. The abdominal weight accumulation, which reflects structural change in fat cell receptor behaviour, responds more slowly over eight to twelve weeks of sustained cortisol normalisation.
What is the difference between high cortisol and low cortisol symptoms?
High cortisol produces a wired but exhausted pattern: anxiety, poor sleep with 3am waking, abdominal weight gain, and immune suppression despite feeling activated. Low cortisol, which can follow prolonged HPA overactivation depleting adrenal output, produces the opposite: flat affect, low motivation, exhaustion from waking, and an inability to respond to demands. Both reflect HPA axis dysregulation and both require restoring the mineral reserves that power the regulation mechanism as the foundation of recovery.
ONE MORE THING BEFORE YOU GO If something in this post resonated but also left a question unanswered, leave it in the comments below. We read every comment and respond with what the research says. We are not asking you to engage for the sake of it. We are giving you a direct line to a researched answer on anything this post did not fully close. If a specific symptom, a specific experience, or a part of the mechanism did not land clearly for your situation, tell us. That is useful information and you will get a direct response. |
Scientific References
- Chandrasekhar, K., Kapoor, J. and Anishetty, S. (2012). A prospective, randomized double-blind, placebo-controlled study of safety and efficacy of a high-concentration full-spectrum extract of ashwagandha root in reducing stress and anxiety in adults. Indian Journal of Psychological Medicine, 34(3), 255-262.
- Choudhary, D., Bhattacharyya, S. and Joshi, K. (2017). Body weight management in adults under chronic stress through treatment with ashwagandha root extract. Journal of Evidence-Based Complementary and Alternative Medicine, 22(1), 96-106.
- Firoz, M. and Graber, M. (2001). Bioavailability of US commercial magnesium preparations. Magnesium Research, 14(4), 257-262.
- Lopresti, A.L., Smith, S.J., Malvi, H. and Kodgule, R. (2019). An investigation into the stress-relieving and pharmacological actions of an ashwagandha extract. Medicine, 98(37), e17186.
- Pickering, G., Mazur, A., Trousselard, M., Bienkowski, P., Yaltsewa, N., Amessou, M., Noah, L. and Pouteau, E. (2020). Magnesium status and stress: the vicious circle concept revisited. Nutrients, 12(12), 3672.
- Prasad, A.S. (2008). Zinc in human health: effect of zinc on immune cells. Molecular Medicine, 14(5-6), 353-357.
- Wienecke, E. and Nolden, C. (2016). Long-term HRV analysis shows stress reduction by magnesium intake. MMW Fortschritte der Medizin, 158(Suppl 6), 12-16.
Legal Disclaimer
The information in this post reflects Penantia’s interpretation of available scientific research and is intended for educational purposes only. It does not constitute medical advice, diagnosis, or treatment. If you are experiencing persistent symptoms including significant mood changes, severe fatigue, or unexplained weight changes, consult a qualified healthcare provider.
Contents
Subscribe to Our Blog
Never Miss any Updates From Blog!




